
Research Line
Neuro-immunology: The neurovascular unit in health and disease
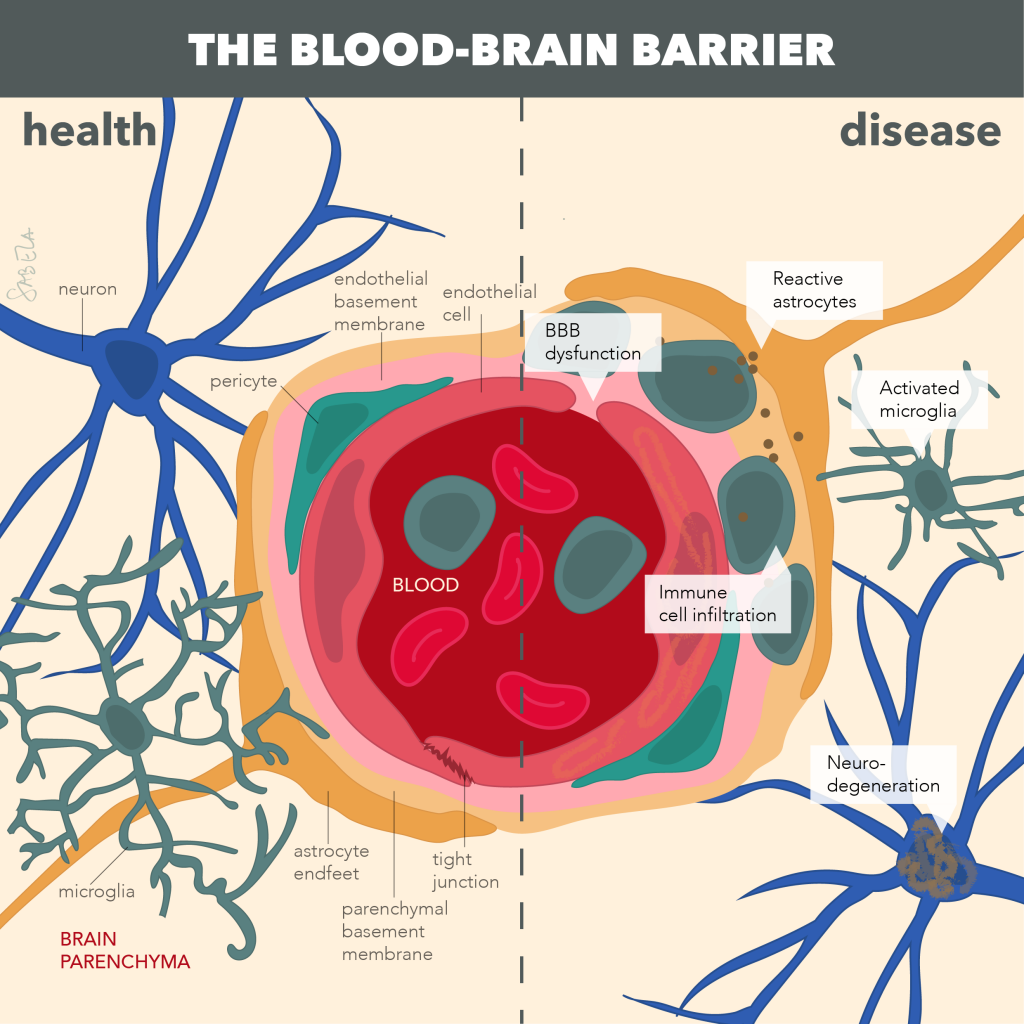
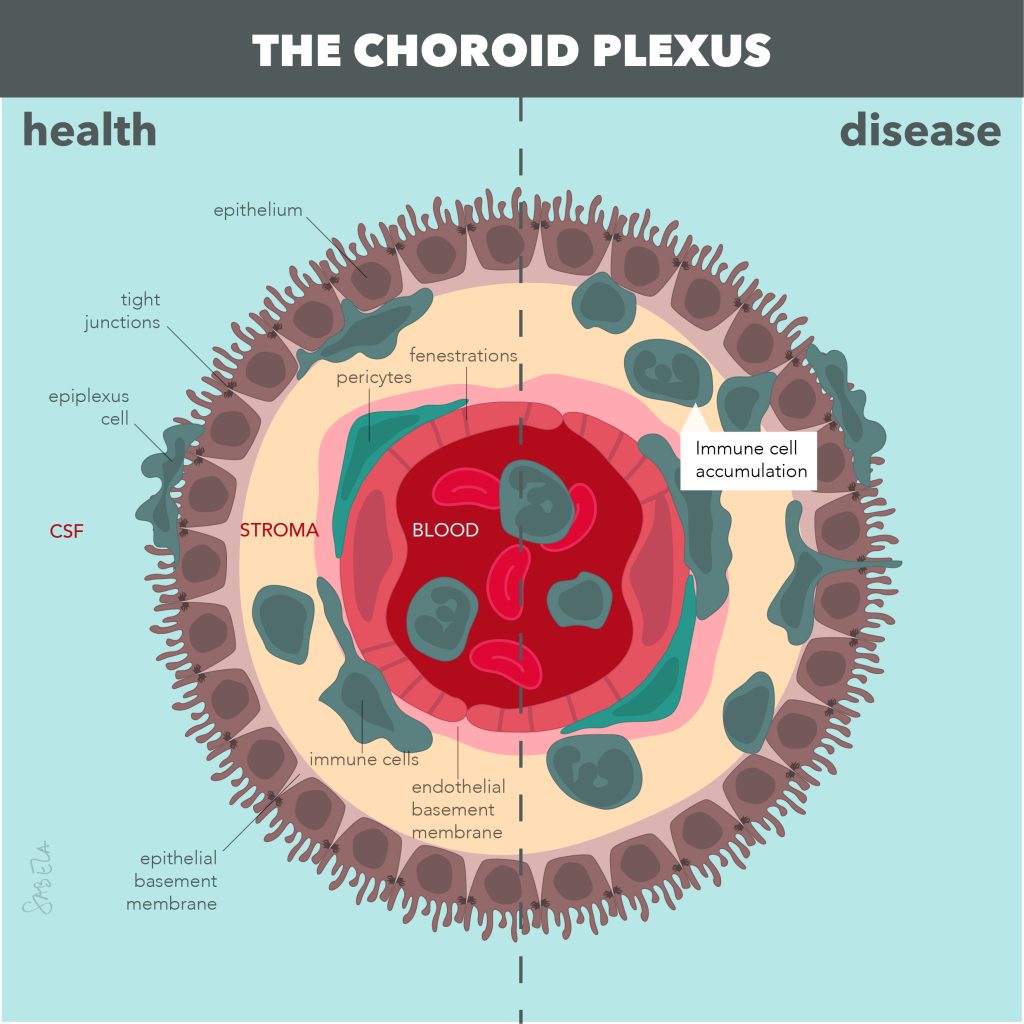
Altered activation of the immune system, neuroinflammation (marked by activated astrocytes and microglia), and dysfunction of the neuro-protective brain barriers are pathological hallmarks of many neurodegenerative disorders, such as multiple sclerosis (MS), various forms of dementia, including Alzheimer’s disease (AD), and stroke. It becomes increasingly clear that chronic neuroinflammation, an altered immune response and neurovascular dysfunction may even be causal for onset and progression of such cognitive disorders, but underlying mechanisms remain unknown. The translational research of the De Vries group is therefore focused on understanding how alterations at the level of the immune system and the brain barriers underlie neuroinflammatory and neurodegenerative conditions. In the current research, we aim to define underlying pathways that initiate neuro-inflammation as potential targets for treatment and identify if such alterations may serve as biomarkers for disease in well-defined patient cohorts. A better understanding of such pathological processes may in future not only lead to new diagnostic tools that reflect ongoing neuro-inflammation and brain barrier dysfunction, but may also lead to potential novel intervention strategies to fight neurogical disorders.
Key publications
- van Olst L, Coenen L, Nieuwland JM, Rodriguez-Mogeda C, de Wit NM, Kamermans A, Middeldorp J, de Vries HE. Crossing borders in Alzheimer’s disease: A T cell’s perspective. Adv Drug Deliv Rev. 2022 Sep;188:114398. doi: 10.1016/j.addr.2022.114398. Epub 2022 Jun 30.PMID: 35780907
- Rodríguez-Lorenzo S, van Olst L, Rodriguez-Mogeda C, Kamermans A, van der Pol SMA, Rodríguez E, Kooij G, de Vries HE. Single-cell profiling reveals periventricular CD56brightNK cell accumulation in multiple sclerosis. 2022 May 10;11:e73849. doi: 10.7554/eLife.73849.PMID: 35536009
- Wevers NR, Nair AL, Fowke TM, Pontier M, Kasi DG, Spijkers XM, Hallard C, Rabussier G, van Vught R, Vulto P, de Vries HE, Lanz HL. Modeling ischemic stroke in a triculture neurovascular unit on-a-chip. Fluids Barriers CNS. 2021 Dec 14;18(1):59. doi: 10.1186/s12987-021-00294-9.PMID: 34906183
- Rodríguez-Lorenzo S, Ferreira Francisco DM, Vos R, van Het Hof B, Rijnsburger M, Schroten H, Ishikawa H, Beaino W, Bruggmann R, Kooij G, de Vries HE. Altered secretory and neuroprotective function of the choroid plexus in progressive multiple sclerosis.Acta Neuropathol Commun. 2020 Mar 19;8(1):35. doi: 10.1186/s40478-020-00903-y.PMID: 32192527
- Wouters E, de Wit NM, Vanmol J, van der Pol SMA, van Het Hof B, Sommer D, Loix M, Geerts D, Gustafsson JA, Steffensen KR, Vanmierlo T, Bogie JFJ, Hendriks JJA, de Vries HE. Liver X Receptor Alpha Is Important in Maintaining Blood-Brain Barrier Function.Front Immunol. 2019 Jul 31;10:1811. doi: 10.3389/fimmu.2019.01811. eCollection 2019.PMID: 31417573
Group members

Carla Rodriguez Mogeda, MSc
PhD student
My research focuses on understanding meningeal inflammation in progressive multiple sclerosis. I am specifically interested in the role of B cells, in how they get to the meninges and how they might interact, directly or indirectly, with other immune cells such as microglia. To do this, I use different single-cell techniques for proteomics and transcriptomics, and confocal and multispectral microscopy..

Chaja van Ansenwoude, MSc
PhD student
My research is focused on the role of NK cells in MS pathogenesis, specifically CD56bright NK cells. This cell population appears to accumulate in the brain of MS patients and exhibits an immunomodulatory and migratory phenotype, suggesting a protective role for these cells in MS. We aim to further unravel the mechanisms underlying CD56bright NK cell effector function by studying cellular interactions, immunoregulatory and neuroprotective capacities, mechanisms of migration, and correlations with clinical markers. For this, I will make use of multispectral microscopy, single cell mass cytometry, in vitro BBB and BCSFB models, and co-culture experiments.

Hannah van der Stok, MSc
Research technician
My work focuses on blood brain barrier functioning. I am specifically interested in a protein named FHL2, which potentially plays a role in blood brain barrier dysfunction. Intracellular mechanisms involved in this process are investigated using in vitro models with lentiviral modifications and various molecular assays.

Henrique Nogueira Pinto, MSc
PhD student
My research is centered on the development of a brain-on-a-chip, combining iPSC-derived cerebral organoids and a bioengineered blood-brain barrier (BBB). This platform will be used to assess the capability of certain compounds to cross the BBB and their neurobiological effects, either in a healthy or disease-specific context.

Inge Mulder, PhD
Senior postdoctoral researcher
My research is focused on the inaccurate reperfusion of the microvasculature of the brain, after recanalization therapy (thrombolysis or thrombectomy) in acute ischemic stroke.
I aim to unravel underlying pathophysiological mechanisms of this phenomenon in order to find new therapeutic strategies to improve treatment efficacy. To do this, I use a translational approach including pre-clinical in-vivo 2-photon microscopy, MRI and Mass spectrometry as well as clinical data.

Merel Rijnsburger, PhD
Post-doctoral researcher
Studying the role of hormones in MS pathophysiology

Nienke de Wit, PhD
Postdoctoral researcher
My research focuses on the blood-brain barrier in health and disease on a
molecular level. Using in vitro cell systems and post-mortem human brain
tissue I try to understand specific pathways that are necessary for maintaining
proper barrier function.

Parand Zarekiani, MSc
PhD student
My research focuses on leukodystrophies, which are genetic disorders that primarily affect the brain white matter. More specifically, I study how the neurovascular unit is involved in these diseases. In the past years, the neurovascular unit has been overlooked in leukodystrophies, while it can have significant implications in the disease progression and in treatments. Using a multidisciplinary approach, I collaborate with pathologists, clinicians and biologists in order to unravel the underlying mechanisms in these diseases. For these studies, I use human post-mortem tissue, in vivo and in vitro approaches.

Ruud Fontijn, PhD
Researcher
My work focuses on the blood-brain barrier, in particular on the endothelial component thereof. Mechanisms of blood-brain barrier failure in neurodegenerative diseases are assessed using in vitro models, impedance measurements, lentiviral genetic modification and various biochemical and molecular biological techniques.

Susanne van der Pol, Ing
Research Technician
Expertise in cell isolations, iPSC, cell-based assays, immunostainings (IHC, ICC, IF), CyTOF, FACS.










